 DOI: 10.1302/2058-5216.Ī systematic physical examination should be performed in order to identify any associated injuries involving the ipsilateral foot, knee or other locations in cases of polytrauma. High-energy pilon fractures management: state of the art. Definitive decision making is mostly dependent on the fracture pattern, condition of the soft-tissues, the patient’s profile and surgical expertise.Ĭite this article: Tomás-Hernández J. No single method of fixation is ideal for all pilon fractures, or suitable for all patients. All of this information is crucial for pre-operative planning, incision placement and articular surface reduction. The axial cuts from the CT scan images are essential in order to define the location of the main fracture line, the fracture pattern (sagittal or coronal) and the number of fragments. 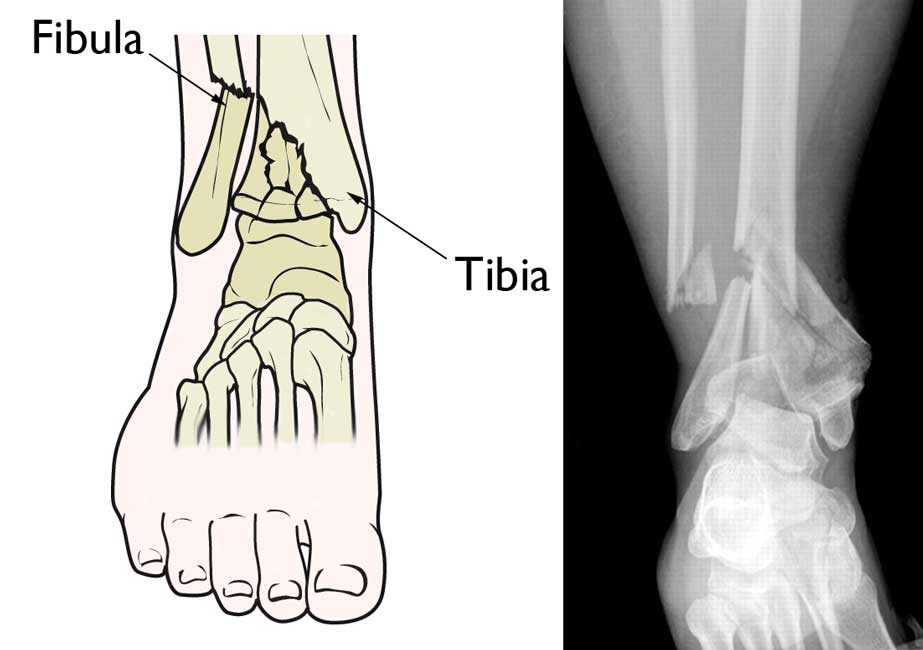
In high-energy fractures with soft-tissue compromise, a staged treatment is generally accepted as the best way to take care of these devastating fractures and is considered a local ‘damage control’ strategy. The current management and recommendations for treatment will be reviewed in this article.Īnatomical reduction of the fracture, restoration of joint congruence and reconstruction of the posterior column with a correct limb axis minimising the soft-tissue insult are the key points to a good outcome when treating pilon fractures.Įven when these goals are achieved, there is no guarantee that results will be acceptable in the mid-term due to the frequent progression to post-traumatic arthritis. Multiple options are described for the definitive surgical management of these fractures, but there is no level I evidence for optimal management. In addition, a novel classification scheme is described to guide recognition and treatment of this fracture pattern.High-energy pilon fractures are challenging injuries. Our results following fixation of this fracture pattern are comparable with results in the literature. The posterior pilon fracture is a challenging fracture pattern to treat, and it has unique characteristics that require careful attention to operative technique. Four complications required operative intervention 2 patients reported continued pain secondary to development of CRPS. Five of 7 patients demonstrated ankle and hindfoot range of motion within 5 degrees of the uninvolved extremity. 
Anatomical reduction of the plafond was noted radiographically in 7 of 11 patients, with the remainder demonstrating less than 2 mm of articular incongruity. Our mean postoperative AOFAS ankle/hindfoot score was 82. Patient records were reviewed to evaluate for secondary complications or operative procedures. 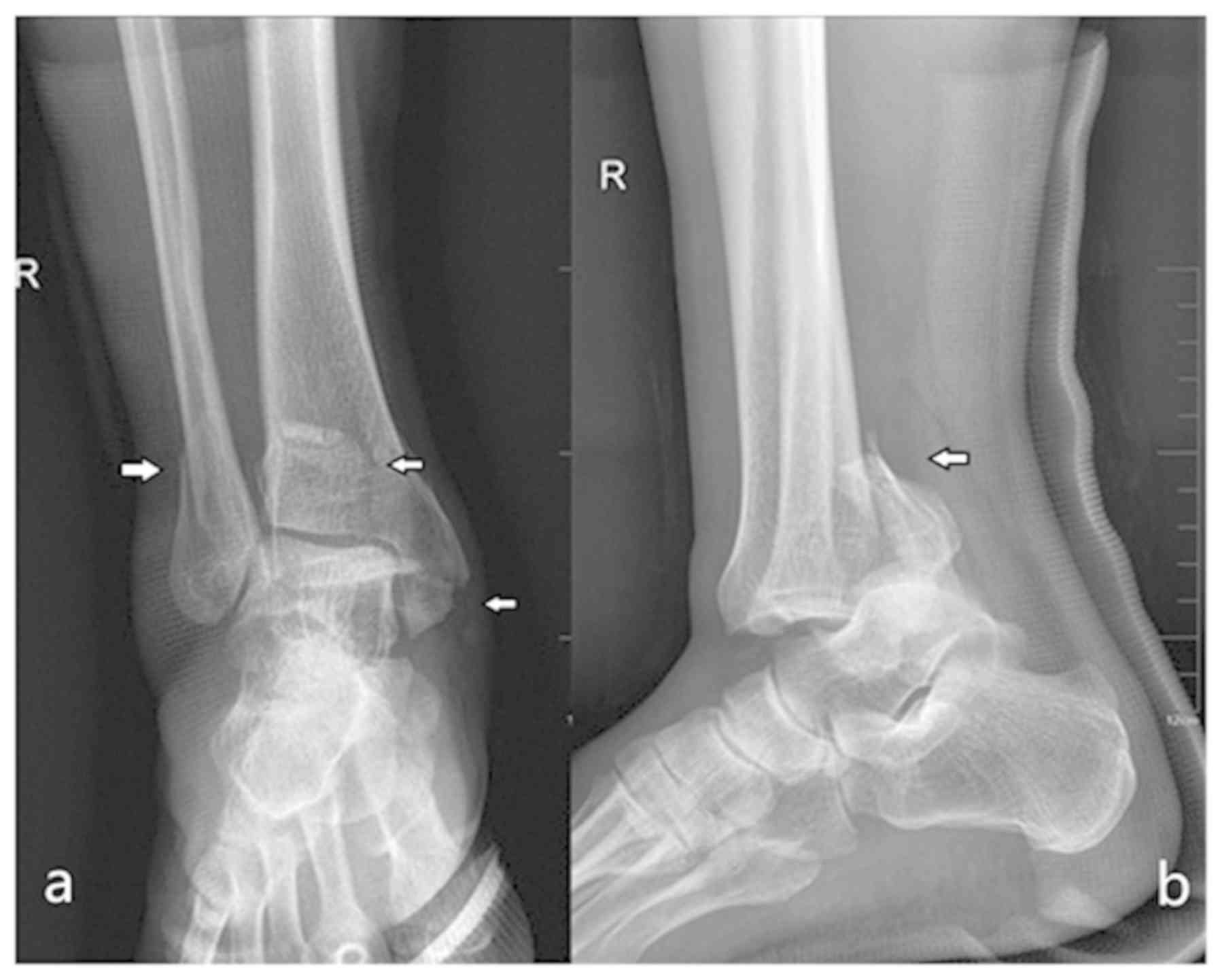
The purpose of this study was to report our outcomes following fixation of this posterior pilon fracture and to describe a novel classification system to help guide operative planning and fixation.Įleven patients were identified following fixation of a posterior pilon fracture over a 4-year span 7 returned at minimum 1-year follow-up to complete a physical examination, radiographs, and RAND-36 (health-related quality of life score developed at RAND as part of the Medical Outcomes Study) and American Orthopaedic Foot & Ankle Society (AOFAS) ankle/hindfoot questionnaires. Failure to identify this fracture pattern has led to poor clinical outcomes and persistent talar subluxation. Fractures that involve the posteromedial plafond extending to the medial malleolus have been described previously in small case series. Posterior malleolus fractures occur in 7% to 44% of ankle fractures and are associated with worse clinical outcomes. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
